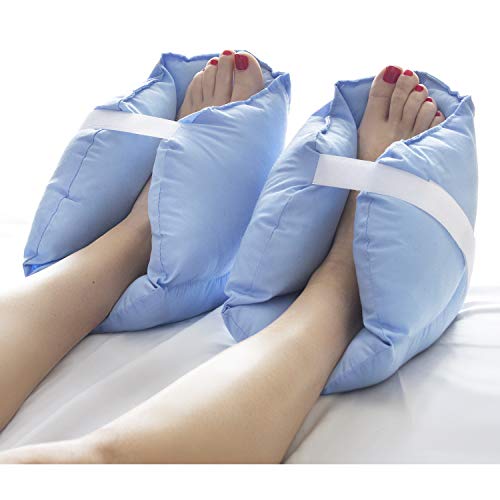
How to Prevent and Manage Pressure Sores Effectively

Disclosure: Some links may be affiliate links. If you buy an item via links on our site, we may earn a commission. Learn more.
For the bed bound, and for the infirm, pressure sores/ulcers can be an all too common problem. It is estimated that just in the US alone, $11 billion per year is spent on treating pressure sores.
Pressure sores can not only be extremely painful, but if left untreated, they can become infected and lead to severe complications including in some cases amputation and death. While pressure sores commonly occur for users with decreased mobility, there are a number of ways in which they can be prevented.
In this article, we will explain how to manage pressure sores, minimize the risk of developing them, and we will cover the best pressure relief equipment that can be used by wheelchair and bed bound users.
What are Pressure Sores/Ulcers?
A pressure sore also known as a bedsore or decubitus ulcer is a skin ulcer. They are formed when pressure is applied to the skin for prolonged periods, causing the blood supply to be cut off to the affected area and causing the skin and underlying tissue to break down and die (atrophy).
Pressure sores commonly occur in situations where the user is confined to a bed or chair/wheelchair for extended periods and is unable to alter position regularly.

If left untreated, pressure sores can be painful and they can be particularly serious especially if an open wound forms and becomes infected.
Common Location of Pressure Sores
Pressure sores commonly occur in areas of the body where the bone is nearer to the surface of the skin and are therefore more prone to excessive pressure from a supporting surface such as a bed, chair or wheelchair.
The location of pressure sores can vary depending on whether the user is lying regularly, for example if they are bed-bound or whether they are sitting for extended periods in the case of a wheelchair user.
For wheelchair users or for anyone that needs to sit for prolonged periods of time, pressure sores are most common in the following areas:
- Heels and at the back of the legs
- Buttocks and Coccyx (tailbone)
- Elbows and back of the arms
- Spine and shoulder blades
- Back of head

For bed bound users, pressure sores are more likely to form in the following areas:
- Heels, ankles and knees
- Hip
- Base of spine such as the sacrum
- Buttocks
- Elbow
- Shoulder and shoulder blades
- Back of head
- Ears (in particular for lateral sleepers)

Common Causes of Pressure Sores
Pressure sores can be caused by any of the following factors:
Pressure
This is where prolonged pressure is applied to a particular area of the user’s body causing the blood supply to cut off, and causing tissue damage. Pressure damage usually occurs when a user has to sit or lay down for extended periods and is unable shift position regularly.
Pressure damage can occur in a number scenarios such as:
- A paralyzed user who uses a wheelchair and is unable to feel any sensation in their lower body and is unable to shift positon when sitting.
- A bed-bound user with impaired mobility who does not have an adjustable bed and relies on a carer to help with being repositioned.
Shearing
Shearing occurs when the skin and deeper tissue are pulled in opposite directions which can result in damage to the deeper tissue and blood vessels.
Common examples of shearing can include:
- When a patient’s adjustable bed is elevated too high at the top section causing them to slide down the bed resulting in their skin being stretched.
- If a user has been repositioned incorrectly in an armchair causing their skin on their back to pinch as they slide down the backrest.
Friction
This is when the user’s skin rubs against a surface causing damage to the epidermis which can then lead to pressure sores.
Examples of friction can include:
- When a user is repositioned incorrectly in bed and their body is pulled along the bed sheets instead of lifted.
- When the user’s heels rub against the bed sheets.
- When a user is transferred from a chair to wheelchair incorrectly causing their arms to rub against the armrests.
Stages of Pressure Sore Development
Pressure sores are graded on a 1 to 4 scale. Each stage relates to the amount of tissue damage the pressure ulcer has caused. Stage 1 being less severe while stage 4 being the most severe type of skin ulcer.
The 4 stages of a pressure sore include:
Stage 1
During the first stage of a pressure sore, there will often be no superficial wound but the skin may feel itchy and painful and heat may be noted in the specific area. The skin may feel firmer or softer than the surrounding skin and discoloration can occur in the affected area which can include red spots for lighter skin tones or purple/blue spots for darker skin tones.
If pressure is applied to the affected area with a finger, and the skin does not stay white, this is an early indication that a pressure sore may be forming.

TIP:
If a pressure sore is only identified in the later stages, it can lead to a serious infection which may hamper recovery times. It is therefore imperative to catch and deal with one early on. If one is identified in the early stages (stage 1 or stage 2), ensure that the user regularly changes position and avoids sitting or lying on the affected area to alleviate pressure. This will assist with recovery and reduce the likelihood of it ulcerating.
Stage 2
During stage 2, damage to the top tissue (epidermis) or underlying tissue (dermis) may occur. A shallow blister or open wound may start to form. If a pressure sore is identified in stage 2, always seek medical assistance in order to avoid the risk of it forming into a higher stage ulcer.
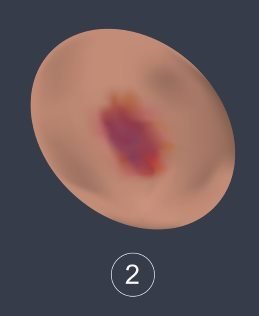
Stage 3
During stage 3, damage to the top tissue (epidermis) and underlying tissue (dermis) and subcutaneous fat occurs causing a deeper wound to form which exposes further layers of skin and muscle. The tendons and bones however are not affected.

WARNING:
Seek immediate medical assistance with stage 3 or stage 4 ulcers especially if the user is experiencing a fever or pus is coming out of the wound or it smells bad. The wound will usually need to be cleaned regularly by a trained medical professional. In some occasions dead or infected skin tissue may also need to be removed and surgery may be required.
Stage 4
In stage 4, a large wound will form causing damage to the skin, muscle, tendons and it may extend all the way down to the bone.

The skin tissue may also begin to die and there is a severe risk of infection which could cause a number of complications including the need of amputation and in some occasions it can be life-threating.

Who’s Most at Risk of Pressure Sores?
Pressure sores can affect a number of users including:
Users with Pre-Existing Medical Conditions
Conditions such as heart disease, diabetes and vascular diseases like dementia and Parkinson’s that impairs blood flow can increase the risk of tissue damage and make a user more vulnerable to pressure sores.
Users with Impaired Mobility
Individuals who suffer with impaired mobility or are bed-bound that may need to spend prolonged periods of time in bed or sitting down in a wheelchair or chair. If the user is unable to change position regularly they are more susceptible to pressure injuries.
They can also suffer from shearing and friction injuries if they are repositioned or transferred incorrectly by a carer or loved one.

Underweight and Overweight Individuals
If a user is underweight, there is less padding over the bonier areas which can increase the risk of pressure related injuries. Dehydration can also cause the skin to become dry which can lead to skin injuries caused by friction and shearing.
Obesity can cause a person to be less active and increased weight can exert greater pressure on the user’s body when sitting or lying down leading to a higher probability of pressure sores.
Incontinent Sufferers
Excessive moisture through incontinence and sweating can cause the skin to become irritated which can result in friction and shearing related injuries.
If the user is not changed or cleaned regularly, urine or faeces can also lead to a build-up of bacteria on the skin which can cause any open wounds to become infected.
People with Limited or No Sensation
Users suffering with paralysis or for those who cannot feel pain in certain parts or all of their body may struggle to feel any discomfort when lying or sitting for prolonged periods. This can lead a person being unaware that they need to change position and they may also fail to notice that they have developed pressure sores.
The Elderly
As a person ages, their skin losses its elasticity and it becomes thinner and more fragile. Thinner skin can bruise and tear more easily and it can also take longer for skin injuries to fully heal.
Due to reduced muscle mass and thinner skin, seniors are more vulnerable to pressure sores especially for those suffering with impaired mobility who may lead a more sedentary lifestyle.
Tips to Help Prevent Pressure Sores
Regular Repositioning
Getting the user to regularly change position when lying on sitting down is especially important in order to help redistribute pressure on their limbs and help reduce pressure sores.
If the user has sufficient mobility, get them to change position every couple of hours if they are lying down. If the user has impaired mobility and is unable to do so, help them with the task.
Manual handling and transfer aids can make repositioning and transferring safer and they can help to prevent any shearing related injuries. A slide sheet can be used to assist with repositioning a user in bed. If the patient is particularly heavy, a hoist can be used instead. Transfer boards can be used to assist someone to transfer to and from a wheelchair to a bed or chair.

Pillows and foam wedges can be used to help relieve pressure in key areas that are susceptible to pressure sores such as the heels, ankles, hips, coccyx, elbows or shoulder blades. If for example, the user is put on their side while in bed, place a pillow between their legs in order to prevent their knees and ankles from touching each other. For increased pressure relief, a memory foam or air-filled mattress can be used which helps to distribute the person’s weight evenly.
Avoid elevating the user’s head above a 30-degree angle if they are lying down, this could otherwise exert greater pressure on the user’s hips and coccyx and it could increase risk of pressure sores.
For anyone sitting for prolonged periods, get them to shift their weight every 15 minutes. Always make sure they adopt a good seating posture. Check that the armrest is at the correct height and ensure their back is straight when seated with their buttocks positioned close to the back of the chair or wheelchair. If the user is slouching, there is an increased risk that they could slide down causing shearing related injuries. A foam or gel seat cushion can also be used on a wheelchair or chair which can help to reduce pressure on the skin.
Skin Care
Inspecting the patient’s skin regularly is imperative. Check their skin daily for any obvious signs of pressure, friction or shearing injuries such as blisters, cuts, abrasions, bruises or open wounds over bony places.
Check that there is no changes in skin tone and that the affected area does not feel warmer or colder to the touch than the surrounding tissue. If the wound smells, this is an indication that it may have become infected therefore always seek medical assistance urgently.
When helping to wash someone, avoid scrubbing their skin, use a soft sponge or wash cloth. If they have sensitive skin, use a pH balanced body wash that will be less harsh. When drying them, gently pat them with a towel and avoid rubbing as this may cause friction injuries.
If the user suffers from incontinence, make sure that their clothes and bedclothes are changed and the skin cleaned and dried immediately. Barrier ointment can prove useful for incontinence sufferers. When the ointment is applied, it acts as impermeable barrier on the skin which can help to protect and prevent irritation and infections.

Eat Healthily
Having a balanced diet and staying hydrated is important especially for the infirm or those who are bed-bound or suffer with impaired mobility. Eating nutritious meals can boost someone’s immune system and it can help to keep infections at bay and assist with wound healing.
If someone is underweight, they will have less cushioning in their bony areas so they will be more susceptible to pressure sores. Regularly weigh the user, and keep a log to ensure that their weight remains steady.
Wear Comfortable and Loose Fitting Clothing
Tight clothing can prove uncomfortable for anyone that is confined to a bed or spends prolonged periods sitting down. Friction injuries due to wearing restrictive clothing can increase the risk of pressure ulcers.
Ensure that the individual wears loose fitting clothing, including underwear and avoid tight socks. Trousers, skirts and tops that have buttons, studs, zippers or thick seams that may dig into the user’s body and prove uncomfortable should be avoided.
When the user is laying or sitting down, ensure that their clothing and any bedding is not ruffled up as these can cause pressure injuries as well.
Exercise Regularly
Encouraging the patient to carry out regular exercise if they have sufficient mobility to do so is important.
As we age, muscle strength and bone density deteriorates, performing exercise on a regular basis can help in delaying this deterioration and it can help to improve blood flow and flexibility.
Strength exercises are beneficial in particular for seniors as this can help in making their muscles stronger thus improving upper and lower body strength. This means they will be able to reposition themselves more easily without requiring assistance which can help to prevent pressure sores. For the bedridden, leg lifts, arm lifts and side rolls can also prove beneficial and help with circulation and muscle strengthening.

Best Pressure Relief Equipment for the Bedridden & Wheelchair Users
Memory Foam Mattress
Unlike a traditional pocket sprung mattress, a memory foam mattress moulds to the contours of a patient’s body.
It helps to evenly distribute the user’s weight over a larger surface thus helping to relieve pressure which can assist in reducing the occurrence of pressure sores.
Gel Mattress
One of the drawbacks of a foam mattress is it can make you hot as it can retain more heat over other types of materials. If you have tendency to sweat in bed, you may want to opt for a gel memory mattress instead.
A gel mattress works in the same way as a foam mattress does, the difference however is gel can help dissipate heat so it remains cooler. Excessive moisture through sweating can increase the risk of friction sores which can lead to ulcers so a gel mattress can reduce heat build-up and help to keep you cooler.
Alternating Air Mattress
Alternating air mattresses contain air pockets that automatically inflate and deflate regularly using a powered pump in order to relieve pressure points on the body.
As the mattresses helps to redistribute the patient’s weight regularly, it can reduce the need of regularly having to manually reposition the person so it can reduce the workload for the carer.
Mattress Topper
A cheaper alternative to purchasing a pressure relieving mattress is to opt for a mattress topper/overlay instead. A mattress topper fits onto an existing mattress and it can provide the user with enhanced comfort.
Mattress toppers can be constructed from a range of pressure relieving materials including, gel, foam, wool and some are air filled.
The following gel memory foam mattress topper from Milliard is reasonably priced and is ideal to help relieve pressure for anyone that needs to spend prolonged periods in bed. The topper has an egg crate texture which helps to distribute points of contact with the user’s body to alleviate any pressure.
The memory foam moulds to the user’s body which helps to maximize comfort and relieve stress. The topper has a cooling gel layer which helps to regulate temperature which means it won’t get too hot. The memory foam is also hypoallergenic and has anti-microbial properties so it’s suitable for anyone with asthma or allergy sufferers.
Profiling/Hospital Bed
One of the drawbacks of a traditional bed for anyone with impaired mobility is they have to rely on a carer or loved one to help them to turn or be repositioned in bed.
A profiling bed however can allow the user to adjust their position and elevation independently to their specific needs with a touch of a button in order to help them maximize comfort and relieve pressure. As a profiling bed is divided into a number of sections, different parts of the bed can be adjusted such as the headrest, backrest and footrest.
Heel Protector
A heel protector is a type of foot and heel guard that protects the user’s feet from excessive pressure when lying down. They fit around the feet and it helps to elevate the user’s heels off the mattress thus helping to reduce the risk of pressure sores from developing.
Most heel protectors are adjustable so they will fit most foot sizes. They are constructed from a range of different pressure relieving materials such as foam, polyester, air-filled and wool.
The following heel protectors from DMI easily fit onto the feet and are adjustable with the simple to use hook and loop Velcro straps. They are made from polyester fibrefill providing enhanced comfort without causing any irritation. The covers are machine washable so they can easily be washed.
Blanket lifter
A blanket lifter is a metal frame that inserts between the bed base and mattress and it is designed to keep the bedsheets/blankets off the user’s legs and feet helping to alleviate any pressure.
The use of a blanket lifter is ideal for anyone that has particularly sensitive skin. It can assist in stopping the bedding from causing any irritation or friction injuries and it allows a person to rest in total comfort.
Most blanket lifters are width adjustable so they are suitable for all sized type beds.
Bed Wedge
Bed wedges are usually constructed from foam and they are a type of positioning aid that can be used to relieve pressure in particular parts of the body that are vulnerable to pressure sores. For example, a wedge can be placed under the tailbone, shoulders or feet and ankles to relieve stress on the body and allowing the person to alternate between different positions.
Wheelchair/Chair Pressure Relief Cushion
For those who use a wheelchair or need to spend prolonged periods sitting down, a gel or foam cushion can prove beneficial.
They are designed to distribute pressure evenly so it can assist in relieving pressure on the user’s back and tailbone when seated.
When deciding on a pressure relief cushion, always check the dimensions to ensure that it will fit in the wheelchair or chair.
The following pressure relief cushion from Vive has a liquid gel core which provides exceptional comfort. The cover is machine washable and the base is non-slip which will keep it stable and secure. The top layers are also waterproof so it’s suitable for incontinence sufferers.
Inflatable pressure cushions are also available that can be inflated and deflated to the specific needs of the user.